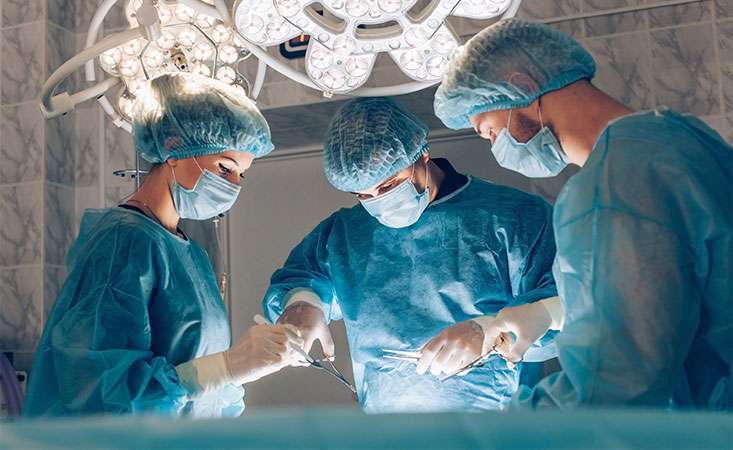
For eligible patients, surgery is the best option for long term survival of pancreatic cancer. Data show high volume surgeons at high volume hospitals have greater success rates and fewer complications. The Pancreatic Cancer Action Network (PanCAN) strongly recommends you have a high volume pancreatic surgeon (more than 15 surgeries per year) perform the surgery.
Below are five more key facts about pancreatic cancer surgery.
- About 20 percent of pancreatic cancer patients are eligible for surgery at diagnosis. Since pancreatic cancer symptoms are often vague and the pancreas is located deep within the body, the disease is often diagnosed in its later stages.
In addition, a significant number of patients who are eligible for surgery are told they are ineligible. PanCAN strongly recommends you see a surgeon who performs a high volume of pancreatic surgeries (more than 15 per year) to determine eligibility.
- There are different types of surgeries that a pancreatic cancer patient can undergo. The most common surgery is known as the Whipple procedure (pancreaticoduodenectomy). The Whipple is performed on patients whose tumor is confined to the head of their pancreas.
Pancreatic cancer patients may also undergo a distal pancreatectomy or complete pancreatectomy, which involve removing some or all of their pancreas. The appropriate surgery is selected based on the size and location of the tumor within the patient’s pancreas and other eligibility criteria.
- Surgery may be offered alongside other treatments. Pancreatic cancer patients may receive chemotherapy and/or radiation or other treatment types before surgery, known as neoadjuvant therapy, or after surgery, known as adjuvant therapy.
- The tissue removed during surgery can help inform future treatment decisions. If you are eligible for surgery, PanCAN strongly recommends calling PanCAN Patient Services to discuss the benefits of molecular profiling.
Tissue taken during surgery (or from a biopsy) can be molecularly profiled to identify the changes in genes and proteins that are present in a patient’s tumor. There are some tumor characteristics, known as “actionable alterations,” that can predict a patient’s response to certain types of treatments.
- Surgery can be supportive (palliative), too. Palliative procedures are performed to alleviate (palliate) symptoms. They do not involve the complete removal of the tumor. Palliative procedures may relieve symptoms of jaundice, pain or nausea and vomiting that are caused by blockage of the bile duct and/or duodenum.
The most common palliative procedures for pancreatic cancer are biliary bypass surgery, gastric bypass surgery and biliary or duodenal stent insertion.
Check out our recent Surgical Advances for Pancreatic Cancer educational webinar.















