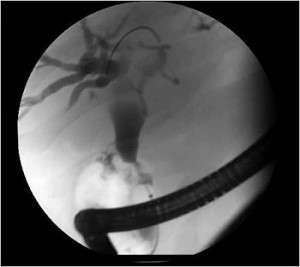
Image courtesy of Shawn Mallery, MD, and Minnesota Pancreas and Liver Center
On This Page:
- What Is Endoscopic Retrograde Cholangiopancreatography (ERCP)?
- Why Use ERCP?
- How Does ERCP Compare with Other Imaging Tests?
- Before the ERCP
- During the ERCP
- After the ERCP
- Side Effects
What Is Endoscopic Retrograde Cholangiopancreatography (ERCP)?
Endoscopic retrograde cholangiopancreatography (ERCP) is a procedure used to get pictures of the digestive tract, including the pancreas. It takes X-ray pictures after a dye is injected through a thin tube. Doctors may use this imaging test to diagnose pancreatic cancer or to treat its symptoms.
ERCP is usually done in a hospital or same-day surgery center.
Why Use ERCP?
In pancreatic cancer, doctors use ERCP to:
- Detect pancreatic cancer
- Get a biopsy (tumor samples for examination)
- See if something, like a tumor, is blocking the pancreas or bile duct
- Treat jaundice
ERCP for Jaundice
Jaundice is a yellowing of the skin and eyes caused by bilirubin (a substance in bile) building up in the body. This can happen if a tumor blocks the bile flowing from the gallbladder into the small intestine.
During an ERCP, the doctor can place a small plastic or metal tube, called a stent, into a blocked bile duct to keep it open and allow bile to flow. Because an ERCP is less invasive than surgery, it is the preferred way to treat jaundice caused by a blockage.
Contact PanCAN Patient Services for more information about jaundice or other pancreatic cancer symptoms and side effects.
How Does ERCP Compare with Other Imaging Tests?
Doctors usually do an ERCP when other tests don’t show pancreatic lesions or when the patient has jaundice.
If a stent is not needed to treat jaundice, a patient can get magnetic resonance cholangiopancreatography (MRCP) instead of ERCP. An MRCP is less invasive than an ERCP.
If doctors only need bile duct images, they may order a percutaneous transhepatic cholangiography (PTC) instead of an ERCP.
For more information about pancreatic cancer diagnosis and these tests, contact PanCAN Patient Services.
Before the ERCP
 The healthcare team gives the patient instructions before an ERCP.
The healthcare team gives the patient instructions before an ERCP.
- The patient cannot eat or drink anything six hours before the procedure.
- Some patients get medicine before the procedure to lower their risk of infection.
- The doctor tells the patient whether to keep taking any medicines before the procedure.
Before the procedure, the patient gets sedative medicine through a vein in the arm to help them relax and painkiller medicine for the throat to block pain. Patients should prepare to have someone else drive them home after the procedure.
During the ERCP
During an ERCP, patients lie on their side. The doctor passes a thin, lighted tube, called an endoscope, through the patient’s mouth, esophagus and stomach and into the small intestine. The patient can breathe normally.
The doctor puts a narrower plastic tube, called a catheter, through the endoscope. Then the doctor adds a contrast dye, a substance that helps doctors see inside a patient’s body more clearly, through the catheter and takes an X-ray picture.
The patient may feel drowsy during the ERCP but stays awake during the procedure.
Usually the procedure lasts 30 – 90 minutes. Most patients find it only mildly uncomfortable.
After the ERCP
After the ERCP procedure is complete, the patient stays in the recovery room until the sedative medicine wears off.
Patients usually go home the same day. The patient should not drive a vehicle after receiving a sedative. Sometimes, patients stay in the hospital one night for observation after the ERCP procedure.
Patients often feel full or the need to pass gas after the procedure. Also, they may have changes in bowel habits, such as soft stool. The healthcare team instructs patients on eating and drinking after an ERCP procedure.
Side Effects
Complications from ERCP are uncommon. About 5 – 7 percent of patients experience inflammation of the pancreas, called pancreatitis, after the procedure. Often the pancreatitis is mild, but it can be serious.
Other rare complications include:
- Gastrointestinal bleeding
- Tearing
- Allergic reactions to anesthesia medicines
- Infection
We’re Here to Help
For more information about pancreatic cancer diagnosis, contact PanCAN Patient Services.
Other Imaging Tests
Endoscopic Ultrasound (EUS)
Computed Tomography or Computerized Axial Tomography (CT or CAT)
Positron Emission Tomography Computed Tomography (PET-CT)
Magnetic Resonance Imaging (MRI)
Information reviewed by PanCAN’s Scientific and Medical Advisory Board, who are experts in the field from such institutions as University of Pennsylvania, Memorial Sloan-Kettering Cancer Center, Virginia Mason Medical Center and more.
Information provided by the Pancreatic Cancer Action Network, Inc. (“PanCAN”) is not a substitute for medical advice, diagnosis, treatment or other health care services. PanCAN may provide information to you about physicians, products, services, clinical trials or treatments related to pancreatic cancer, but PanCAN does not recommend nor endorse any particular health care resource. In addition, please note any personal information you provide to PanCAN’s staff during telephone and/or email communications may be stored and used to help PanCAN achieve its mission of assisting patients with, and finding cures and treatments for, pancreatic cancer. Stored constituent information may be used to inform PanCAN programs and activities. Information also may be provided in aggregate or limited formats to third parties to guide future pancreatic cancer research and education efforts. PanCAN will not provide personal directly identifying information (such as your name or contact information) to such third parties without your prior written consent unless required or permitted by law to do so. For more information on how we may use your information, you can find our privacy policy on our website at https://www.pancan.org/privacy/.





