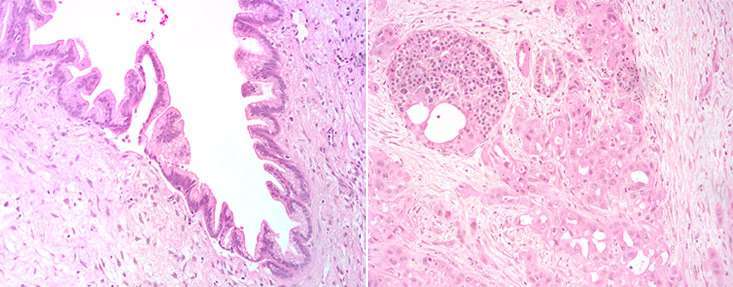
Stained cells from a patient's IPMN (left) and adjacent cancer in their pancreas (right). Images provided by Dr. Laura Wood.
When a cyst is detected in someone’s pancreas, the first priority is characterizing the type of cyst – and determining its likelihood to progress to cancer. If it’s seen as benign, doctors may opt to monitor it over time and not proceed with any treatment. On the other hand, if it’s deemed likely to progress to an invasive cancer, then surgery is typically recommended.
While this is already a highly complex (and potentially emotionally taxing) decision, new research suggests that characterizing the cyst doesn’t tell the whole story.

Laura Wood, PhD
“Our study focused on cysts called intraductal papillary mucinous neoplasm, or IPMN,” explained Laura Wood, PhD, assistant professor of pathology and oncology at the Sol Goldman Pancreatic Cancer Research Center, Johns Hopkins University School of Medicine. “We found an unexpectedly high rate of co-occurring carcinomas [cancers] in the same patients’ pancreas – independent from the IPMN.”
Published in the journal Gut earlier this month, the paper emphasizes the importance of analyzing the entire pancreas, rather than focusing on a particular cyst that has been detected.
“Screening based on the molecular features of that IPMN (such as from cyst fluid) may miss the high-risk alterations in an independent carcinoma,” Wood said. “Our results suggest that screening methodologies should try to assay the entire pancreas, not just the known cyst.”
Included among the authors of the Gut paper is Michael Goggins, MD, professor of pathology at the Johns Hopkins University School of Medicine, and principal investigator of one of the inaugural $1 million Research Acceleration Network (RAN) grants from the Pancreatic Cancer Action Network (PanCAN), funded to honor the legacy of Skip Viragh.
Goggins and his team focus on analyzing pancreatic juice, fluid within the pancreas that may contain valuable clues about cysts or early cancerous lesions that may be present. Wood pointed out that analysis of pancreatic juice is a “good candidate” for whole-pancreas screening, but she adds that further testing is necessary to determine its value instead of, or in addition to, direct analysis of cyst fluid.
“Our data suggest a ‘whole-pancreas’ screening approach is important due to the biology of IPMNs and co-occurring cancers, but they do not specifically address which samples are best for screening. These studies need to be done in the future,” Wood added.
If you have questions about analyzing cysts or qualifications to join a pancreatic cancer high-risk screening study, contact PanCAN Patient Services.
Wood’s collaborative study was made possible by funding from the federal government as well as private funders. She shared that she “cannot overstate the importance” of private funding sources, like PanCAN’s Research Grants Program, for the success of pancreatic cancer research in her lab and in the field overall.
“Such private funding has been absolutely critical to almost every major advance in pancreatic cancer research,” she said. “My research group could never have succeeded without private funding to bridge me from my start-up funds to federal grant support.”
She added: “Also, such funds continue to form a critical component of our lab’s funding, particularly for highly innovative projects.”
To allow PanCAN to continue to fund leading-edge research projects and to offer innovative clinical initiatives for patients, please donate today.
















