On This Page:
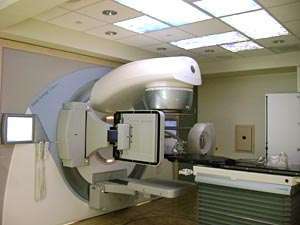
Image courtesy of Elekta Synergy and Johns Hopkins University
- What Is Radiation Therapy?
- When Is Radiation Used to Treat Pancreatic Cancer?
- Types of radiation therapy for pancreatic cancer
- Will I Get Chemotherapy with Radiation Therapy?
- Where Do I Get Radiation Therapy?
- What Are the Side Effects of Radiation Therapy?
- Radiation Therapy Video
What Is Radiation Therapy?
Radiation therapy is a cancer treatment that uses high-energy radiation, in the form of waves (like x-rays) or particles (like protons), to kill cancer cells or stop them from growing and spreading.
During radiation therapy, the patient lays on a table. In most cases, a large machine rotates around the table and directs the radiation through several places around the stomach area into the pancreatic tumor.
The goal of radiation is to treat the tumor to keep it from growing or coming back (recurring), while sparing the healthy organs or tissue nearby.
Radiation works to kill cancer cells in the tumor. In some cases, this can possibly shrink the tumor.
Since radiation therapy is directed to a specific (focused) area, it is a localized treatment.
When Is Radiation Used to Treat Pancreatic Cancer?
Radiation therapy may be used in all stages of pancreatic cancer.
Patients Whose Tumors Can Be Removed by Surgery (Resectable)
In patients with resectable tumors, radiation can be given:
- Before surgery (neoadjuvant), to lower the risk of leaving cancer cells behind and to lessen the chance of the cancer coming back after surgery
- After surgery (adjuvant), to help prevent the cancer from returning and to kill tiny cancer cells that may have been left behind (positive margin or nodes)
When patients have borderline resectable pancreatic cancer, radiation therapy is often given before surgery to prevent recurrence.
Patients Whose Tumors Cannot Be Removed by Surgery (Unresectable)
Patients with unresectable tumors may also receive radiation therapy. In these cases, it is often given to prevent the tumor from growing, which could cause pain or other symptoms.
This may include radiation therapy to:
- Relieve pain caused by the tumor
- Control bleeding (possible if the tumor involves the bowel or stomach)
Types of radiation therapy for pancreatic cancer
There are two main types of radiation therapy: external beam radiation therapy and internal radiation therapy.
External Beam Radiation Therapy
External beam radiation therapy uses a machine outside the body to direct radiation beams through the skin to the tumor or area where the tumor was removed. It is used often to treat pancreatic cancer.
Standard external beam radiation therapy is usually given 5 days a week for 2 – 5 weeks. Each treatment lasts only a few minutes.
There are many options for pancreatic cancer treatment with external beam radiation therapy, alone or with other treatment types. Patients should discuss the treatment options with their radiation oncologists, who are ideally part of a multidisciplinary team.
Pancreatic cancer is a complex disease best evaluated by a team of specialists. An ideal team would include expertise in radiology, gastroenterology, medical oncology, radiation oncology, surgery, pathology, supportive care and nutrition. The Pancreatic Cancer Action Network recommends consulting with a multidisciplinary team whenever possible.
Contact PanCAN Patient Services for a free list of pancreatic cancer specialists and multidisciplinary teams.
 In addition to standard external beam radiation therapy, two methods of planning and delivering external beam radiation may be used to treat pancreatic cancer:
In addition to standard external beam radiation therapy, two methods of planning and delivering external beam radiation may be used to treat pancreatic cancer:
- Intensity-modulated Radiation Therapy (IMRT)
- Stereotactic Body Radiation Therapy (SBRT)
These specialized methods lessen the amount of radiation delivered to normal tissues.
Intensity-modulated Radiation Therapy (IMRT)
Intensity-modulated radiation therapy (IMRT) delivers focused radiation to the tumor by changing (modulating) radiation beam strength (intensity) under precise computer control.
It uses 3D computer imaging to figure out the size, shape and location of the tumor. Along with changing the radiation dose’s strength, this:
- Allows a higher dose of radiation to be delivered to the tumor
- Lessens the amount of radiation delivered to healthy tissue near the pancreas
Compared to standard radiation therapy, this may:
- Cause fewer side effects
- Allow higher doses of radiation to be delivered safely
Patients usually receive IMRT treatment 5 days a week for 5 – 6 weeks. Each treatment session usually takes 10 – 30 minutes.
Stereotactic Body Radiation Therapy (SBRT)
Stereotactic body radiation therapy (SBRT) is designed to deliver focused, high doses of radiation in five treatments or less.
SBRT treats the tumor and a very small area beyond it. Nearby organs like the bowel or stomach get low doses of radiation. This may lead to reduced side effects.
Because pancreatic tumors move as patients breathe, with SBRT, the radiation oncology team accounts for tumor motion and may use techniques or equipment so that the beams hit the tumor while sparing healthy tissue.
Research suggests that pancreatic SBRT may be recommended for some patients and is ideally delivered at a high-volume center with experience in this type of radiation.
SBRT is usually given over 1 – 5 sessions within 2 weeks. Each treatment session lasts 15 – 60 minutes.
MRI-Guided Radiation Therapy
Magnetic Resonance Imaging (MRI) guided radiation therapy is a type of radiation treatment that uses images taken by an MRI machine throughout treatment to direct radiation directly to a tumor, minimizing damage to healthy tissues, like nearby stomach or bowel.
During treatment, the machine takes several MRI pictures per second, and the beam of radiation can follow the tumor as it moves with a person’s breathing or digestion, which can significantly change the location of a tumor within the body as the lungs expand or as the stomach and intestines fill and empty. This technology can “adapt” the radiation plan in near real-time to re-focus the radiation on the tumor and away from healthy tissues. Some studies have reported that this approach may result in better tumor control and less side effects.
Since MRI guided radiation therapy can deliver more targeted doses of radiation, some people may receive less treatments.
Only a few manufacturers produce the machine required for this kind of treatment, called an MRL or MR-linac (MRI-linear accelerator.) Since this is a newer therapy, it is not yet widely available. This type of radiation therapy continues to be studied to determine its efficacy and safety in treating patients with pancreatic cancer.
There are several ongoing clinical trials taking place evaluating MRI-guided radiation therapy, for a personalized clinical trial search, or information on institutions that offer this therapy, contact a Case Manager.
Internal Radiation Therapy
Internal radiation therapy (brachytherapy) delivers radiation through radioactive material inserted in or near the cancer.
This type of radiation therapy is rarely used in pancreatic cancer patients except as part of a clinical trial.
Will I Get Chemotherapy with Radiation Therapy?
Patients may get radiation therapy alone or in combination with chemotherapy, known as chemoradiation.
When chemotherapy is given with radiation, a lower dose of chemotherapy is usually used. Chemotherapy acts as a “radiosensitizer” that can improve the radiation’s effect on the tumor.
The chemotherapy drugs most commonly used with radiation therapy are:
- 5-Fluorouracil (5-FU)
- Capecitabine (Xeloda®)
- Gemcitabine (Gemzar®)
5-FU is used most often since there is more experience using it in combination with radiation and there are usually fewer side effects.
Clinical trials are studying different types of radiation therapy in combination with chemotherapy or investigational therapies like immunotherapy.
More clinical trials are needed to determine radiation therapy’s effectiveness both alone and with other therapies.
Where Do I Get Radiation Therapy?
Radiation therapy is usually an outpatient treatment. Patients do not usually stay overnight in the hospital. Patients go either to the hospital or to an outpatient clinic. Radiation may also be used in a clinical trial setting.
Both IMRT and SBRT are practiced mainly in high-volume centers. Contact PanCAN Patient Services for a free list of high-volume centers with specialized experience.
Patients should speak with their healthcare team about any treatment decisions, including radiation therapy. Response to treatment is individual, and a doctor will be able to better provide information about eligibility, benefits versus risks, and next steps.
What Are the Side Effects of Radiation Therapy?
Side effects differ depending on the type of radiation therapy given. The most common side effects of radiation therapy for pancreatic cancer are:
- Loss of appetite
- Nausea
- Diarrhea
- Fatigue
Mild skin redness is possible but not common in pancreatic cancer treatment.
Radiation therapy treatments do not hurt during the procedure. Patients may feel some abdominal discomfort toward the end of the treatment series, but the actual treatment session is not painful.
The effects of radiation therapy can build up over time. They usually peak 4 – 5 weeks after the first treatment and go away 1 – 2 weeks after treatment is over.
Patients should avoid ibuprofen during and after radiation therapy, as it can raise the risk of getting an ulcer.
If patients have pain in the stomach area, black stools or other side effects after radiation therapy, tell the radiation oncologist. A healthcare professional can prescribe medicines or supportive care accordingly.
PanCAN Patient Services also has a free educational booklet for more information about supportive care.
Radiation Therapy Video
We’re Here to Help
For free, in-depth and personalized resources and information on pancreatic cancer treatment or anything else related to the disease, contact PanCAN Patient Services.
Related Topics
-
Chemotherapy
Get information about the most common form of pancreatic cancer treatment.
-
Treatment Types
Learn about pancreatic cancer treatment options.
-
Clinical Trials
See why pancreatic cancer patients should consider clinical trials.
-
Specialists
Find out why seeing a specialist improves outcomes and how to find one.
-
Communicating with Your Healthcare Team
Learn how to improve discussions with your doctors.
Information reviewed by PanCAN’s Scientific and Medical Advisory Board, who are experts in the field from such institutions as University of Pennsylvania, Memorial Sloan-Kettering Cancer Center, Virginia Mason Medical Center and more.
Information provided by the Pancreatic Cancer Action Network, Inc. (“PanCAN”) is not a substitute for medical advice, diagnosis, treatment or other health care services. PanCAN may provide information to you about physicians, products, services, clinical trials or treatments related to pancreatic cancer, but PanCAN does not recommend nor endorse any particular health care resource. In addition, please note that any personal information you provide to PanCAN’s Case Managers during telephone and/or email communications may be stored and used to help PanCAN achieve its mission of assisting patients with, and finding cures and treatments for, pancreatic cancer. Stored constituent information may be used to inform PanCAN programs and activities. Information also may be provided in aggregate or limited formats to third parties to guide future pancreatic cancer research and treatment efforts. PanCAN will not provide personal directly identifying information (such as your name or contact information) to such third parties without your prior written consent unless required or permitted by law to do so.





