On This Page:
- What Is Positron Emission Tomography (PET)?
- Why Use PET?
- How Should You Prepare for a PET Scan?
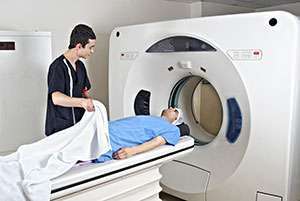
- What Happens During a PET Scan?
- What Happens After a PET Scan?
- Limitations of PET Imaging
- Are PET Scans Covered by Insurance?
What Is Positron Emission Tomography (PET)?
Positron Emission Tomography (PET) is an imaging test that shows how energy is being used in the body. It may be used with other tests to diagnose pancreatic cancer.
Cells need glucose (sugar) for energy. When cells become cancerous, they often change the way they use glucose and need more of it. Growing cells, such as pancreatic cancer cells, use glucose faster than other cells. PET imaging shows this change.
Why Use PET?
PET scans may:
- Find abnormalities before other imaging tests such as computed tomography (CT) or magnetic resonance imaging (MRI) scans
- Help the doctor see extremely small cancerous masses that might otherwise go unnoticed
- Indicate whether the mass is cancerous
- Help the healthcare team figure out the right treatment, including whether surgery is possible
- Show if and where pancreatic cancer has spread
- Help the healthcare team monitor how a tumor is responding to treatment
How Does PET Imaging Compare to Other Imaging Tests?
PET imaging tracks how organs and tissues are working. CT and MRI images provide information on structures inside the body, such as their size, shape and location.
For pancreatic cancer diagnosis, CT scans are more common than PET scans. A PET test is usually used with CT or MRI tests.
PET scans are more sensitive and useful in some cancers than others. Studies are still looking at the PET scan’s usefulness in pancreatic cancer.
Until it has proven to be the best imaging test for pancreatic cancer, it is important to use PET scans with other imaging tests to build a complete picture of a patient’s cancer.
For more information about these tests and their uses, contact PanCAN Patient Services.
PET-CT Scan
Some hospitals and centers have a machine that combines PET and CT scans. This allows radiologists to use both procedures’ strengths.
In pancreatic cancer, studies show that the combined PET-CT scan is more successful than a PET scan alone in deciding if surgery is possible. The combined imaging can also better find pancreatic cancer that has spread to other areas.
PET-CT is not a replacement for high-quality, contrast-enhanced CT or MRI scans. But it may be used along with these tests.
How Should You Prepare for a PET Scan?
PET scans are usually an outpatient procedure. The healthcare team gives the patient detailed instructions on how to prepare.
In general, a patient should not exercise heavily or eat or drink for four hours before the appointment. These activities can affect the pictures.
Patients should wear comfortable, warm clothing since scanner rooms are often cool.
What Happens During a PET Scan?
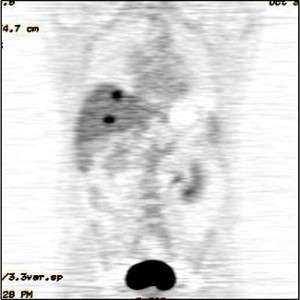
Highlighted areas on PET scan image show presence of cancer cells in the liver.
The most common PET scan type is FDG-PET. For this procedure, a patient gets an injection of fluorodeoxyglucose (FDG), a type of glucose (sugar). As organs and tissues break it down, FDG releases very small amounts of radiation. The PET scanner tracks and records these amounts.
In many imaging tests, patients come into contact with some radiation. Talk to your doctor about the pros and cons of having different scan types.
A computer turns the information into whole-body images that show areas where cancer cells may be. The cancer cells show up as bright or highlighted areas on the PET images.
A PET scan usually lasts two to three hours and proceeds as follows:
- Patients receive FDG through an injection.
- They sit for 45-60 minutes, while the FDG travels through the blood and collects in organs and tissues.
- They must lie still for 15-75 minutes for the scan.
What Happens After a PET Scan?
After a PET scan is complete, the patient should drink water to help flush out the rest of the medical grade substances used for the test.
A radiologist interprets the PET scan results and sends them to the patient’s doctor. Patients should get results within a few business days.
Limitations of PET Imaging
A positive PET scan does not always mean the person has pancreatic cancer. The opposite is also true. A negative PET scan does not always mean the person does not have pancreatic cancer.
PET imaging can give false results if a person’s chemical balances are not normal. For example, pancreatitis (pancreatic swelling), infections and other diseases can cause incorrect results.
Both PET and CT imaging have trouble detecting tumors that are less than one centimeter in diameter. While PET imaging does not always show smaller tumors than CT imaging can find, it may show small tumors that CT imaging misses. The opposite may also be true.
Diabetic patients or patients who eat a few hours before the test can receive incorrect results due to their blood sugar or blood insulin levels. Diabetic patients should ask for specific diet guidelines to control glucose levels during the day they take the test. The glucose used in a PET scan does not harm diabetics.
Are PET Scans Covered by Insurance?
Insurance providers, including Medicare and private insurance companies, cover most PET scan costs. Patients should check with their insurance provider to understand their coverage.
We’re Here to Help
For more information about PET scans, other imaging tests or pancreatic cancer diagnosis, contact PanCAN Patient Services.
Other Imaging Tests
Computed Tomography or Computerized Axial Tomography (CT or CAT)
Magnetic Resonance Imaging (MRI)
Endoscopic Retrograde Cholangiopancreatography (ERCP)
Information reviewed by PanCAN’s Scientific and Medical Advisory Board, who are experts in the field from such institutions as University of Pennsylvania, Memorial Sloan-Kettering Cancer Center, Virginia Mason Medical Center and more.
Information provided by the Pancreatic Cancer Action Network, Inc. (“PanCAN”) is not a substitute for medical advice, diagnosis, treatment or other health care services. PanCAN may provide information to you about physicians, products, services, clinical trials or treatments related to pancreatic cancer, but PanCAN does not recommend nor endorse any particular health care resource. In addition, please note any personal information you provide to PanCAN’s staff during telephone and/or email communications may be stored and used to help PanCAN achieve its mission of assisting patients with, and finding cures and treatments for, pancreatic cancer. Stored constituent information may be used to inform PanCAN programs and activities. Information also may be provided in aggregate or limited formats to third parties to guide future pancreatic cancer research and education efforts. PanCAN will not provide personal directly identifying information (such as your name or contact information) to such third parties without your prior written consent unless required or permitted by law to do so. For more information on how we may use your information, you can find our privacy policy on our website at https://www.pancan.org/privacy/.





